From crisis to catalyst: Mandy Daly on parent advocacy and patient-centred innovation
June 13, 2024
by Mandy Daly
MedTech insights
Parents Perspective
Mandy Daly is the founder of the Irish Neonatal Health Alliance, which works to reduce the incidence of preterm births and to empower families affected by prematurity in Ireland. A medical and disability underwriter, she became a passionate advocate in the neonatal space after her daughter was born preterm in 2006.
Mandy specialises in Advocacy, Education, and Research, contributing to several health system reviews and educational initiatives. She has served on advisory boards for the European Foundation for the Care of Newborn Infants and NIDCAP Federation International since 2012. Mandy has also published papers in journals such as the British Medical Journal and The Lancet.
Her contributions extend beyond Ireland, shaping global conversations on neonatal health. Here, she shares her insights into the progress in supporting parents and infants born preterm, highlighting the importance of a patient-centred approach to medical device innovation and development.
Little did I know that when my daughter Amelia was born at the end of week 25 of my pregnancy in 2006, the grenade, aka preterm birth, that exploded in our lives would be the catalyst for a journey that would see me help shape the landscape of neonatology in Ireland today.
Parenting a preterm child in 2006 was challenging. There was no public awareness around preterm birth. There wasn’t a Model of Care for Neonatal Services in Ireland. The National Neonatal Transport Service (a service that transfers critically ill infants from regional hospitals to tertiary units to receive life-saving medical care) only operated from 9am-5pm. Neonatal education was not available in Ireland. These obstacles forced those interested in pursuing careers in the area to venture abroad to obtain further education. Research into preterm birth in the Irish context was in its infancy, and those affected by preterm birth did not have a voice in the advocacy, education, health or research arenas. On a personal level, the emotional, psychological, physical and educational support that we as a family required to navigate the journey of preterm birth successfully was not available.
The Irish Neonatal Health Alliance (INHA), a multi-stakeholder, multi-disciplinary collaborative platform, grew out of my own unmet needs. Following Amelia’s birth, my observations and lived experience told me that innovation within the neonatal space in Ireland was happening in silos. The pillars that underpin the work of the INHA include advocacy, awareness, education, research and support. Today, the organisation continues to expand its services largely based on the journeys of many of our families. Eighteen years later, these families are still living with the legacy of preterm birth.
Preterm birth is for life, not just the Neonatal Unit, and everything that happens in the Neonatal Unit can have an effect—positive, negative or cumulative.
In those very early days, when Amelia was clinging to life on a ventilator, I could never have imagined the impact that her preterm birth would have on her life, on our lives as a family and on the Irish neonatal landscape. Not a single day passes without preterm birth raising its head in some form or other, be it through her sensory processing issues, her developmental coordination disorder, her avoidant restrictive food intake disorder, her health anxiety, her executive functioning issues, her circulatory issues, her respiratory health issues, or her emotional regulation issues.
And then, there are the unknown entities: the health issues that are lying dormant that research tells us can arise in adults born preterm. That “ticking time bomb” never really goes away, but rather than wallow in the “what might be”, I have embraced the opportunities my situation has afforded me. Preterm birth informs every aspect of my work as an educator, an embedded patient researcher, a peer supporter, and an advocate.
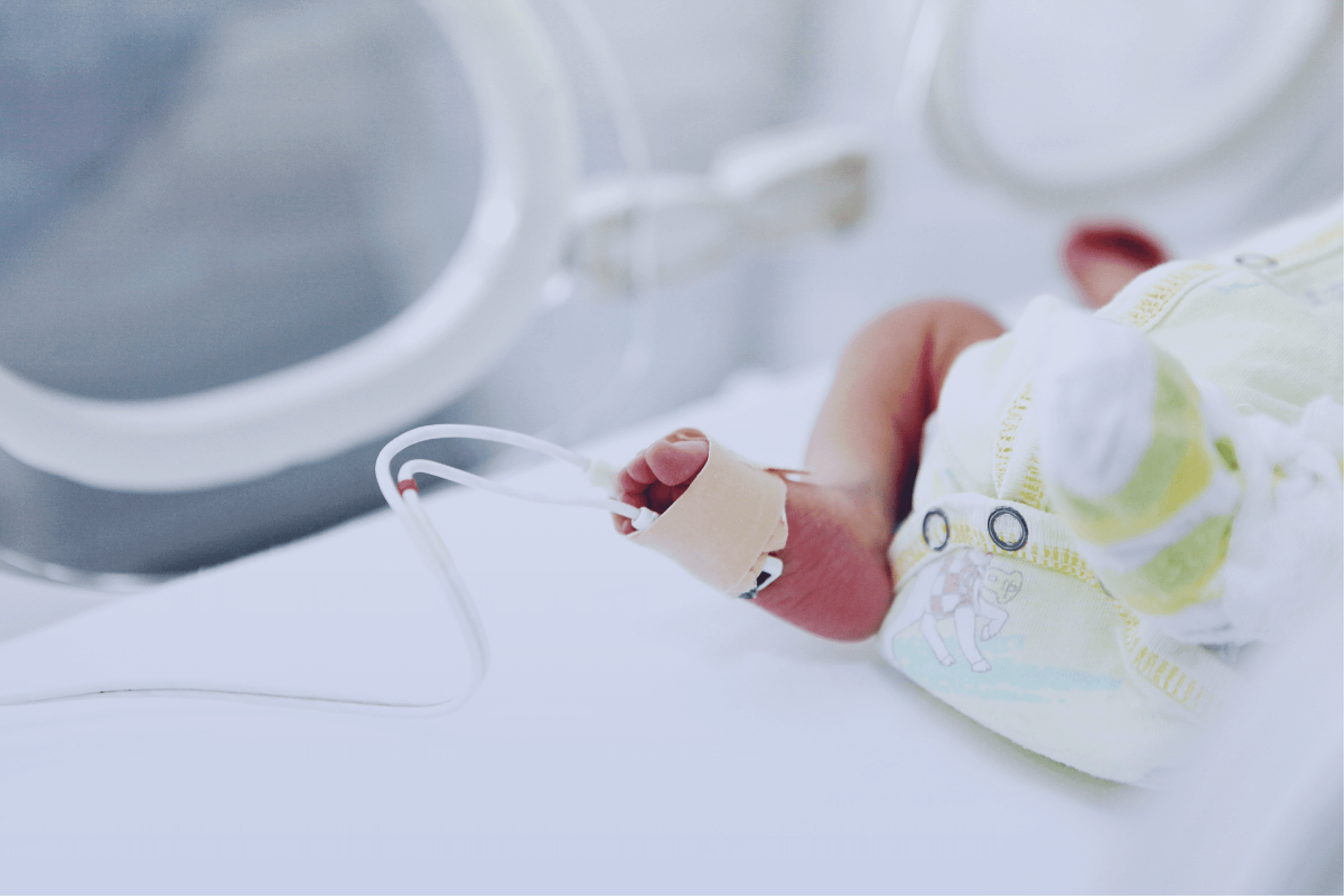
Journey to family-centred, developmentally supportive neonatal care
In 2006, our preterm infants were a silent and unheard community. No one really understood their challenges or unmet needs. The social care and health services developed for preterm infants were devised without their consultation. Well-intentioned academics and investigators carried out research but without consideration for the meaningfulness of the research. Healthcare providers were educated about the community but did not hear about the lived experience during their training programmes. The outcomes of babies born preterm were not captured anywhere.
Fast forward to 2024 and we have a Model of Care for Neonatal Services in Ireland. We have a Neonatal Transport Service that operates 24 hours a day. Mothers affected by a preterm birth can now avail of extended maternity leave. Family-centred and developmentally supportive care is fast becoming the norm in our neonatal units. Healthcare education programmes now embed the patient’s lived experience into their curricula. Patients from the affected community develop and deliver education to stakeholders.
Neonatal research is guided and steered by those affected by preterm birth. The patient community works closely with funding agencies to ensure that neonatal research addresses the unmet needs of the cohort. Patient families have a voice in the research ethics space where they assess the ethical soundness of research in the field and sit at the medicines regulation table. No longer are clinical guidelines developed without consulting the neonatal patient community—clinical audits are conducted in collaboration with us and the patient voice is at the heart of health technology assessments that happen in the field. The patient journey is told through a unique lived experience lens that draws large audiences to medical conferences across the globe.
The importance of embracing research, innovation and technology
In the dynamic world of healthcare, technological advancements are transforming patient care and treatment methods. Medical devices are integral to healthcare delivery, supporting diagnosis, treatment, and monitoring of medical conditions. Their versatility and efficacy contribute to improved patient outcomes and enhanced quality of care, and they play a critical role in advancing personalised medicine by enabling tailored interventions and therapies based on individual patient characteristics.
Medical device manufacturing is a complex landscape that requires the harmonious collaboration of various disciplines. From concept to production, multi-disciplinary collaboration plays a vital role in developing safe, effective, and innovative medical devices that ultimately save patient lives and enhance patient’s quality of life.
Medicines development and neonatology rarely appear in the same sentence. The nature of neonatology is such that very few new medicines have been developed in this area over the last thirty years. However, our understanding of preterm birth and its lifelong impact, and our knowledge around events that happen in-utero or at the point of birth that can have devastating effects on the life of the affected individual, have expanded exponentially—largely thanks to the efforts of the research community.
One area gaining momentum in recent years is the use of technology and AI in neonatology. These advancements serve not only to enhance care pathways and improve outcomes but also to bolster health systems that are strained by resource shortages, inadequate funding, and escalating service demands.

Why a patient-centric approach is the future
A patient-centric approach must be at the heart of all medical device manufacturing collaboration.
What does a patient-centric approach look like? Many diverse and varied examples across the medicines and medical device development space of endeavours are classified as patient-centric partnerships. However, true patient-centric partnerships are those where patients are invited to participate as equal partners in the initial exploratory landscape mapping and horizon-scanning conversations. These are conversations where the patient engagement role and responsibilities are clearly defined, clear and concise objectives are outlined, the education requirements of either the patient community or, indeed, the developers/researchers are addressed to facilitate and support true engagement and where there is a clear vision for how patient engagement will be captured, measured, reported and valued.
Successful patient partnerships are based on equity, trust, respect, dignity, transparency and communication.
The importance of listening to the lived experiences of the community for whom a medical device is being developed cannot be overstated. Understanding how a medical condition affects every aspect of a patient's daily life and how their potential is curtailed due to late diagnosis or inadequate access to suitable treatments adds invaluable insight.
It’s often difficult for those operating in the medical device development space to imagine the real-world experience of the end user of the device they are developing. Increasingly, we are seeing this sector embark on journeys of co-creation with the affected communities to explore their challenges, scope the possible solutions and develop devices collaboratively.
Understanding the biology of a disease is no longer sufficient when embarking on creating a new medical device. Bringing firsthand experience to the development table focuses the minds of developers; it transforms the disease and its impact from words on a page to a tangible person. No one is better placed to inform and guide innovation than one who lives, breathes and walks the disease path every day of their life.
Patient-centric collaboration ensures that medical devices are designed not only with cutting-edge technology but with the end user in mind. Multi-stakeholder, multi-disciplinary collaboration accelerates innovation by fostering the exchange of knowledge and insights.
Co-design has a symbiotic benefit for all parties involved in the process. The unmet needs of patients are addressed, treatment pathways are improved, and patient quality of life is improved. Investment in meaningful innovation results in the production of devices that make a real difference to the patient community. By involving patients in the development process from the outset, financial and time wastage can be minimised. Devices co-developed with patients, for patients, hold greater potential for acceptance and compliance within the patient community.
Health systems and society also benefit from the patient-centric approach to device development. If a medical device aids early diagnosis and treatment access or enhances condition monitoring, patient compliance and quality of life see significant improvement. Future health system financial and resource burden is reduced as patient’s future health is preserved by timely access to treatments and better treatment compliance. Improved patient health outcomes facilitate more fruitful and meaningful contributions to society by the patient community, thereby benefiting society as a whole. In doing so, we champion a healthier tomorrow, one device at a time.
“Alone we can do so little, together we can do so much” Helen Keller
See Irish Neonatal Health Alliance for further info & resources: https://www.inha.ie/
Follow Mandy Daly on LinkedIn: https://www.linkedin.com/in/mandy-daly-63425217/